-
Recent Trends in Affordable Care Act Insurance
Health insurers offering Affordable Care Act (ACA) plans must walk a fine line to offer mandated services while remaining profitable. Although ACA included design features intended to protect plans against risks from excess enrollment of unhealthy individuals, such features are insufficient in light of actual plan enrollments, leading some insurers to exit ACA marketplaces and others to experiment with limited-benefit plan designs to hold down costs. Both actions reduce choice for consumers, are detrimental to individuals with costly chronic conditions, and, in some cases, increase litigation risk for insurers offering limited benefits.
Profitability and Enrollment: Full-Benefit versus Limited-Benefit Plans
The ACA requires that plans cover certain essential health benefits and forbids explicit exclusion of individuals with pre-existing health conditions. As a result, plans must attract a mix of individuals with varying health risks such that an average premium results in net profit. The ACA includes a risk-adjustment model intended to limit the financial consequences of attracting participants who are disproportionately unhealthy or healthy by adjusting the effective premium.
In practice, enrollment in ACA plans has included fewer healthy — and more chronically ill — adults than anticipated, and the risk-adjustment model systematically fails to compensate plans for certain types of chronically ill patients. This has forced insurers to raise premiums on full-benefit plans (to avoid large losses), to only offer plans with limited benefit designs, or to exit the exchanges entirely.
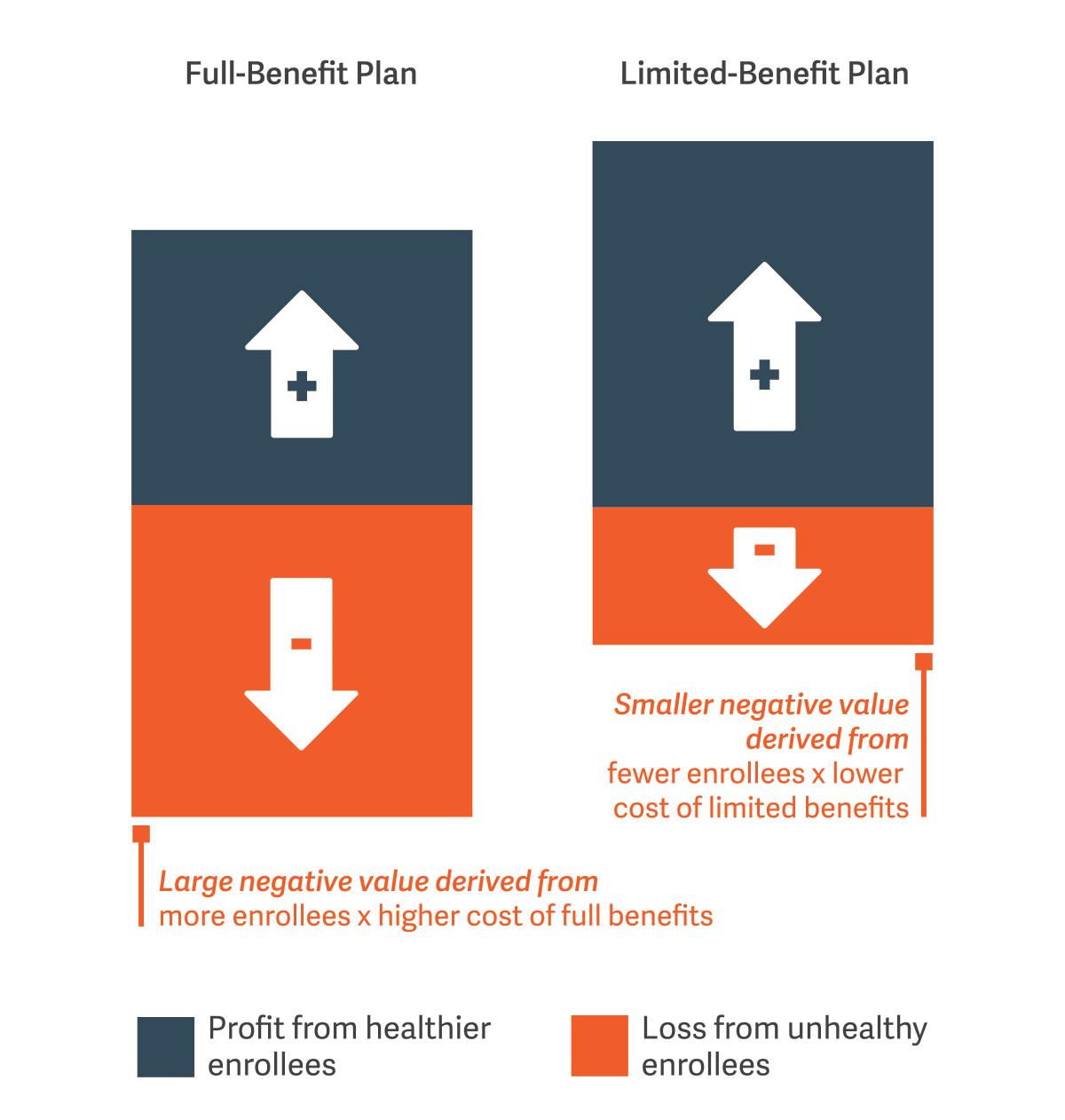
To help contain healthcare costs, ACA permits plans to incorporate patient cost-sharing, narrow provider networks, limits on nonessential services, and restrictive formularies into plan design. However, individuals with chronic conditions may correctly predict that they will face higher total costs under a limited benefit plan and may look elsewhere for coverage. Insurers offering limited benefit plans thus improve profitability directly, by limiting the loss on each unhealthy enrollee, and also indirectly, by attracting fewer such enrollees. (See figure.)
These mechanisms of improved profitability correspond to two types of litigation risk faced by limited benefit plans:
- Enrollees may allege misleading information was provided regarding covered benefits.
- Plans may be perceived as discriminatory towards individuals with chronic illnesses due to the higher cost burden experienced by these individuals.
Future changes to risk adjustment, recently announced by the Centers for Medicare and Medicaid Services, may more appropriately compensate plans that cover individuals with high medical costs. However, changes won’t go into effect until 2018. In the meantime, expect additional insurers to exit the marketplaces rather than face losses or lawsuits. ■
Anita Chawla, Senior Advisor
Adapted from “Following Recent Trends In Affordable Care Act Insurance,” by Anita Chawla and Keziah Cook, published on Law360.com, September 9, 2016.

