-
Leveraging Real-World Evidence to Assess Differences in Management of Chronic Spontaneous Urticaria
Innovative treatments may offer pathways to improve the management of chronic spontaneous urticaria (CSU), but gaps in access to those therapies, variations in disease management, and differences in prescribing patterns persist.
Although antihistamines are the recommended first-line treatment for patients with CSU, the availability of advanced therapies may offer promise to those for whom disease remains uncontrolled following antihistamine use. In the year since the following analysis was conducted, the FDA has approved two new therapies for CSU: dupilumab, a biologic, and rembrutinib, an oral small molecule. The International CSU guidelines have been updated to include all three FDA approved advanced therapies (omalizumab, dupilumab, and remibrutinib) as first line options in antihistamine-refractory patients. Systemic corticosteroid (SC) use may offer short-term relief to such patients; however, clinical guidelines recommend limiting their long-term use due to the risk of adverse events (AEs).
Real-world evidence reveals meaningful differences in treatment patterns and health care utilization among patients with CSU, including variation in access to advanced therapies and reliance on SCs and emergency services.
“Despite poorly controlled disease, only a small proportion of patients were escalated to advanced therapies (biologics), suggesting an unmet need for more effective CSU treatment options.”To assess disparities in treatment, health care resource use (HCRU), and AEs among patients with CSU, we conducted analyses using a large US insurance claims database. Our study was descriptive in nature, and no formal comparisons were performed. Key findings were as follows:
Treatment Differences by Race and Insurance Coverage
Here we assessed the rates of uncontrolled disease and whether there were treatment differences for patients as a function of their race and insurance coverage.
Descriptively, on average, there were notable differences in disease management. For instance, patients who are Black and covered by Medicaid had the highest rates of SC use and emergency room visits among the groups studied. Despite these indicators of greater acute care use, this group also experienced among the lowest rates of biologic initiation, as compared to other groups.
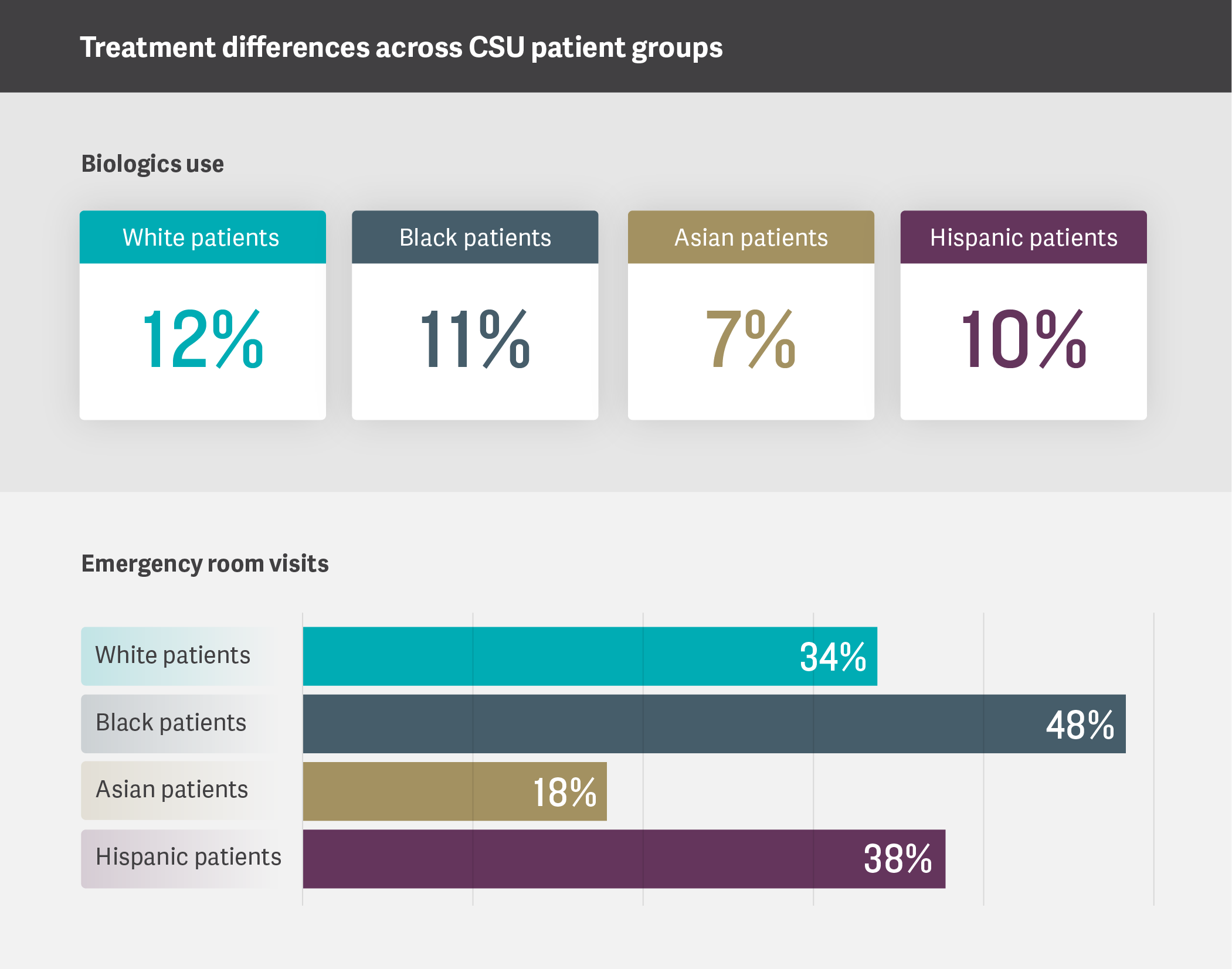
Taken together, these findings suggest that a higher proportion of Black patients with CSU is admitted to emergency rooms for CSU-related issues. This potentially suggests higher rates of uncontrolled disease and a disproportionate disease burden among Black patients with CSU. Furthermore, those patients may not be considered as candidates for advanced, guideline-recommended therapies relative to other patients in clinical practice.
Impact of Specialist Care
In addition to variation across racial and insurance subgroups, our analysis identified descriptive differences in treatment patterns based on specialist involvement. We found that patients with visits to both an allergist and dermatologist received higher proportions of biologic prescriptions, as compared with other groups who saw some combination of primary care physicians and specialists. Of note, patients who saw only an allergist had a higher degree of use of and shorter wait times for advanced therapies.
Across all specialist groups, high levels of SC use and acute care utilization persisted, suggesting ongoing unmet need for more effective and guideline-aligned treatment strategies in CSU management.
Our findings suggest that access to specialists – particularly allergists – appears linked to faster and greater use of advanced therapies.
Risks Associated with SC Use
Lastly, we examined patterns of SC use and related outcomes among patients with CSU. We found descriptive evidence that SC use was associated with the occurrence of AEs such as lipid disorders and hypertension, and prolonged use was generally associated with high proportions of patients with AEs and greater AE-related HCRU.
Although clinical guidelines recommend restricting SCs to short-term rescue use, many patients experience prolonged exposure to them. This underscores the potential clinical and economic consequences of reliance on these therapies and highlights the importance of equitable access to alternative, advanced treatment options.
Conclusion
Our studies indicate that disparities by race and socioeconomic status exist in the management of patients with CSU. Patients with Medicaid – particularly Black patients – appear more likely to rely on emergency care and SCs and less likely to receive advanced biologic therapies. At the same time, high levels of SC use and acute care visits across all populations indicate an unmet need for more effective disease control across patient groups.
Further research in this area is needed to uncover the structural and clinical factors driving disparities and to identify strategies that may help reduce gaps in care. By leveraging the real-world evidence offered by these and other studies, providers, payers, and manufacturers may be better positioned to make treatment decisions and improve equitable access to guideline-recommended therapies for patients with CSU.
Irina Pivneva, Vice President
Jason Doran, Manager
Frédéric Kinkead, AssociateAdapted from three research posters presented during the American College of Allergy, Asthma & Immunology (ACAAI) 2025 Annual Scientific Meeting, including:
Racial, Ethnic, And Socioeconomic Disparities in Chronic Spontaneous Urticaria: A United States Claims Database Study (2025), coauthored by Marc A. Riedl, (University of California, San Diego); Dhaval Patil, Jonathan Rodrigues, Merin Kuruvilla, Panagiotis Orfanos, and Tara Raftery (Novartis); Jason Doran, Irina Pivneva, and Frédéric Kinkead (Analysis Group); and Gil Yosipovitch (University of Miami Miller School of Medicine)
Treatment Patterns in Patients With Chronic Spontaneous Urticaria: Results From a US Claims Database Study (2025), coauthored by Marc A. Riedl, (University of California, San Diego); Dhaval Patil, Jonathan Rodrigues, Merin Kuruvilla, Panagiotis Orfanos, and Tara Raftery (Novartis); Jason Doran, Irina Pivneva, and Frédéric Kinkead (Analysis Group); and Gil Yosipovitch (University of Miami Miller School of Medicine)
Adverse Events Associated With Corticosteroid Use in Chronic Spontaneous Urticaria Management (2025), coauthored by Gil Yosipovitch (University of Miami Miller School of Medicine); Dhaval Patil, Jonathan Rodrigues, Merin Kuruvilla, and Tara Raftery (Novartis); Irina Pivneva, Jason Doran, and James Signorovitch (Analysis Group); and Marc A. Riedl, (University of California, San Diego)
This feature was published in March 2026.
